Chronic obstructive pulmonary disease - adults - discharge
COPD - adults - discharge; Chronic obstructive airways disease - adults - discharge; Chronic obstructive lung disease - adults - discharge; Chronic bronchitis - adults - discharge; Emphysema - adults - discharge; Bronchitis - chronic - adults - discharge; Chronic respiratory failure - adults - dischargeYou were in the hospital to treat breathing problems that are caused by chronic obstructive pulmonary disease (COPD). COPD damages your lungs. This makes it hard to breathe and get enough oxygen.
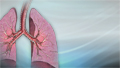
Chronic obstructive pulmonary disease
Chronic obstructive pulmonary disease (COPD) is a common lung disease. Having COPD makes it hard to breathe. There are two main forms of COPD:Chroni...
After you go home, follow instructions on taking care of yourself. Use the information below as a reminder.
When You're in the Hospital
In the hospital you received oxygen to help you breathe better. You may also need to use oxygen at home. Your health care provider may have changed some of your COPD medicines during your hospital stay.
Keep Active
To build strength:
- Walk until it is a little hard to breathe.
- Slowly increase how far you walk.
- Try not to talk when you walk.
- Ask your provider how far to walk.
- Ride a stationary bike. Ask your provider how long and how hard to ride.
Build your strength even when you are sitting.
- Use small weights or an exercise band to strengthen your arms and shoulders.
- Stand up and sit down several times.
- Hold your legs straight out in front of you, then put them down. Repeat this movement several times.
Ask your provider whether you need to use oxygen during your activities, and if so, how much. You may be told to keep your oxygen above 90%. You can measure this with an oximeter. This is a small device that measures your body's oxygen level. Talk with your provider about how much oxygen is safe to use and what oxygen saturation to aim for.
Talk to your provider about whether you should do an exercise and conditioning program such as pulmonary rehabilitation.
Self-care
Know how and when to take your COPD medicines.
- Take your quick-relief inhaler when you feel short of breath and need help fast, but always according to your provider's instructions so you don't take too much.
Quick-relief inhaler
Quick-relief medicines for chronic obstructive pulmonary disease (COPD) work quickly to help you breathe better. You take them when you are coughing...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Take your long-term medicines every day.
Long-term medicines
Control medicines for chronic obstructive pulmonary disease (COPD) are medicines you take to control or prevent symptoms of COPD. You must use these...
Read Article Now Book Mark Article
Eat smaller meals more often, such as 6 smaller meals a day. It might be easier to breathe when your stomach is not full. Do not drink a lot of liquid before eating, or with your meals.
Ask your provider what foods to eat to get more energy.
What foods to eat to get more energy
If you are sick or undergoing cancer treatment, you may not feel like eating. But it is important to get enough protein and calories so you do not l...
Keep your lungs from becoming more damaged.
- If you smoke, now is the time to quit.
Time to quit
There are many ways to quit smoking. There are also resources to help you. Family members, friends, and co-workers may be supportive. But to be su...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Stay away from smokers when you are out, and do not allow smoking in your home.
- Stay away from strong odors and fumes.
- Do breathing exercises.
Talk to your provider if you feel depressed or anxious.
Stay Away From Infections
Having COPD makes it easier for you to get infections. Get a flu shot every year. Ask your provider if you should get a pneumococcal (pneumonia) vaccine, respiratory syncytial virus (RSV) vaccine, a Tdap (tetanus, diphtheria and pertussis) vaccine, a Zoster vaccine and a COVID-19 vaccine.
Flu shot
All content below is taken in its entirety from the CDC Inactivated Influenza Vaccine Information Statement (VIS) www. cdc. gov/vaccines/hcp/current-...

Pneumococcal (pneumonia) vaccine
Content below is taken in its entirety from the CDC Information Statement (VIS): www. cdc. gov/vaccines/hcp/current-vis/pneumococcal-conjugate. html...
Respiratory syncytial virus
All content below is taken in its entirety from the CDC Respiratory Syncytial Virus (RSV) Preventive Antibody Immunization Information Statement (IIS...
Tdap
All content below is taken in its entirety from the Centers for Disease Control (CDC) Tdap Vaccine Information Statement (VIS): www. cdc. gov/vaccine...
COVID-19 vaccine
COVID-19 vaccines are used to prepare the body's immune system to protect against COVID-19. Everyone ages 6 months and older should get a 2025-2026 C...
Wash your hands often. Always wash after you go to the bathroom and when you are around people who are sick.
Stay away from crowds. Ask visitors who have colds to wear masks or to visit when they're all better.
Save Your Energy at Home
Place items you use often in spots where you do not have to reach or bend over to get them.
Use a cart with wheels to move things around the house and kitchen. Use an electric can opener, dishwasher, and other things that will make your chores easier to do. Use cooking tools (knives, peelers, and pans) that are not heavy.
To save energy:
- Use slow, steady motions when you are doing things.
- Sit down if you can when you are cooking, eating, dressing, and bathing.
- Minimize going up and down the stairs.
- Get help for harder tasks.
- Do not try to do too much in one day.
- Keep your phone with you or near you.
- After bathing, wrap yourself in a towel rather than drying off.
- Try to reduce stress in your life.
Going Home With Oxygen
Never change how much oxygen is flowing in your oxygen setup without asking your provider.
Oxygen setup
Because of your medical problem, you may need to use oxygen to help you breathe. You will need to know how to use and store your oxygen.
Always have a back-up supply of oxygen in the home or with you when you go out. Keep the phone number of your oxygen supplier with you at all times. Learn how to use oxygen safely at home.
How to use oxygen safely at home
Oxygen makes things burn much faster. Think of what happens when you blow into a fire; it makes the flame bigger. If you are using oxygen in your h...
Follow-up
Your hospital provider may ask you to make a follow-up visit with:
- Your primary care provider
- A respiratory therapist, who can teach you breathing exercises and how to use your oxygen
- Your lung doctor (pulmonologist)
- Someone who can help you stop smoking, if you smoke
- A physical therapist, if you join a pulmonary rehabilitation program
When to Call the Doctor
Contact your provider if your breathing is:
- Getting harder
- Faster than before
- Shallow, and you cannot get a deep breath
Also contact your provider if:
- You need to lean forward when sitting in order to breathe easily
- It is difficult to speak even a few words without being short of breath
- You are using muscles around your ribs to help you breathe
- You are having headaches more often
- You feel sleepy or confused
- You have a fever
- You are coughing up dark mucus
- Your fingertips or the skin around your fingernails are blue
References
Global Initiative for Chronic Obstructive Lung Disease (GOLD) website. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: 2024 report. goldcopd.org/2024-gold-report/. Accessed May 16, 2024.
Han MK, Lazarus SC. COPD: clinical diagnosis and management. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 6th ed. Philadelphia, PA: Elsevier; 2022:chap 64.
National Heart, Lung, and Blood Institute website. COPD. www.nhlbi.nih.gov/health/copd. Updated October 25, 2023. Accessed May 16, 2024.
Reilly J. Chronic obstructive pulmonary disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 76.
US Department of Veterans Affairs website. VA/DoD Clinical Practice Guideline for The Management Of Chronic Obstructive Pulmonary Disease, Version 3.0. www.healthquality.va.gov/guidelines/CD/copd/VADoDCOPDCPGFinal508.pdf. Updated April 2021. Accessed May 16, 2024.
-
COPD (chronic obstructive pulmonary disorder) - illustration
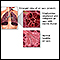
Chronic obstructive pulmonary disease (COPD) refers to chronic lung disorders that result in blocked air flow in the lungs. The two main COPD disorders are emphysema and chronic bronchitis, the most common causes of respiratory failure. Emphysema occurs when the walls between the lung's air sacs become weakened and collapse. Damage from COPD is usually permanent and irreversible.
COPD (chronic obstructive pulmonary disorder)
illustration
-
COPD (chronic obstructive pulmonary disorder) - illustration
Chronic obstructive pulmonary disease (COPD) refers to chronic lung disorders that result in blocked air flow in the lungs. The two main COPD disorders are emphysema and chronic bronchitis, the most common causes of respiratory failure. Emphysema occurs when the walls between the lung's air sacs become weakened and collapse. Damage from COPD is usually permanent and irreversible.
COPD (chronic obstructive pulmonary disorder)
illustration
Review Date: 5/3/2024
Reviewed By: Allen J. Blaivas, DO, Division of Pulmonary, Critical Care, and Sleep Medicine, VA New Jersey Health Care System, Clinical Assistant Professor, Rutgers New Jersey Medical School, East Orange, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.


