Crohn disease - discharge
Inflammatory bowel disease - Crohn disease - discharge; Regional enteritis - discharge; Ileitis - discharge; Granulomatous ileocolitis - discharge; Colitis - dischargeCrohn disease is a disease in which parts of the digestive tract become inflamed. It is a form of inflammatory bowel disease (IBD).
When You're in the Hospital
You were in the hospital because you have Crohn disease. This is an inflammation of the surface and deep layers of the small intestine, large intestine, or both. Less often, other parts of your gastrointestinal tract can be affected.
You may have had exams, lab tests, stool tests, and imaging tests such as CT or MRI. The inside of your colon (large intestine) and ileum (last part of the small bowel) may have been examined using a flexible tube (colonoscopy). A sample of your tissue (biopsy) may have been taken.
You may have been asked not to eat or drink anything and have been fed only through an intravenous line. You may have received special nutrients through a feeding tube.
You may have also started taking new medicines to treat your Crohn disease. Treatment usually involves long-term medicines that blocks the immune system from causing inflammation. This may be by pill , infusion, or injection. These medicines will be continued at home.
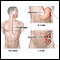
Surgeries you may have had include repair of a fistula, small bowel resection, dilation of a narrowing (called a stricture) or ileostomy.
Small bowel resection
You had surgery to remove all or part of your small intestine (small bowel). You may also have had an ileostomy.
Ileostomy
You had an injury or disease in your digestive system and needed an operation called an ileostomy. The operation changed the way your body gets rid ...
What to Expect at Home
After a flare-up of your Crohn disease, you may be more tired and have less energy than before. This should get better. Ask your health care provider about any side effects from your new medicines. You should see your provider regularly. You may also need follow-up blood and stool tests, especially if you are on new medicines.
If you went home with a feeding tube, you will need to learn how to use and clean the tube and your skin where the tube enters your body.
Feeding tube
Your child's gastrostomy tube (G-tube) is a special tube in your child's stomach that will help deliver food and medicines until your child can chew ...
Clean the tube
A nasogastric tube (NG tube) is a special tube that carries food and medicine to the stomach through the nose. It can be used for all feedings or fo...
Immunosuppressive medicines for IBD can make you at higher risk of getting other infections. Make sure to speak with your provider about getting the appropriate vaccinations to decrease your risk. Live vaccinations are not given while on those medicines, so follow your provider's guidance.
If you are planning to get pregnant in the near future, discuss with your provider. It is best to have your Crohn disease under control (be in remission) before pregnancy.
Diet
When you first go home, you may be asked to drink only liquids or eat different foods from what you normally eat. Ask your provider when you can start your regular diet.
You should eat a well-balanced, healthy diet. It is important that you get enough calories, protein, and important nutrients from a variety of food groups.
Certain foods and drinks can make your symptoms worse. These foods may cause problems for you all the time or only during a flare-up. Try to avoid foods that make your symptoms worse.
- If your body does not digest dairy foods well, limit dairy products. Try low-lactose cheeses, such as Swiss and cheddar, or an enzyme product, such as Lactaid, to help break down lactose. If you must stop eating dairy products, talk with a dietitian about getting enough calcium. Some experts believe that you should avoid dairy products altogether until you are tolerating your regular diet.
- Too much fiber may make your symptoms worse. Try baking or stewing fruits and vegetables if eating them raw bothers you. Eat low-fiber foods if that does not help enough.
- If you have a narrowing of the bowel, you may be put on a low-residue diet. Your provider or a dietitian may be helpful to understand this diet.
- Avoid foods that are known to cause gas, such as beans, spicy food, cabbage, broccoli, cauliflower, raw fruit juices, and fruits, especially citrus fruits.
- Avoid or limit alcohol and caffeine. They may make your diarrhea worse.
Eat smaller meals, and eat more often. Drink plenty of liquids.
Ask your provider about extra vitamins and minerals you may need:
- Iron supplements (if you have iron deficiency anemia). Sometimes iron is given intravenously.
- Nutritional supplements. Because Crohn disease can cause poor absorption, certain vitamin levels may be low and you may need to supplement. Follow your provider's recommendations.
- Calcium and vitamin D supplements to help keep your bones strong.
- Vitamin B-12 shots, to prevent anemia.
Talk with a dietitian, especially if you lose weight or your diet becomes very limited.
Stress
You may feel worried about having a bowel accident, embarrassed, or even feel sad or depressed. Other stressful events in your life, such as moving, job loss, or the loss of a loved one, can cause problems with your digestion.
These tips help you to manage your Crohn disease:
- Join a support group. Ask your provider about groups in your area. The Crohn's and Colitis Foundation of America educates and provides information and supportive services to manage the disease.
- Exercise. Talk with your provider about an exercise plan that is right for you.
- Try biofeedback to reduce muscle tension and slow your heart rate, deep breathing exercises, hypnosis, or other ways to relax. Examples include doing yoga, listening to music, meditation, reading, or soaking in a warm bath.
- See a mental health professional for help if necessary. Having a chronic disease can be difficult and there is no shame in wanting to discuss your feelings with a professional.
Drug Treatment
Your provider may give you some medicines to help relieve your symptoms. Based on how bad your Crohn disease is and how you respond to treatment, your provider may recommend one or more of these medicines:
- Anti-diarrhea medicines can help when you have very bad diarrhea. Loperamide (Imodium) can be bought without a prescription. Always talk to your provider before using these medicines. In particular, do not take antidiarrheal medicines if you have fever, bloody stool, or blockages.
- Fiber supplements may help your symptoms. You can buy psyllium powder (Metamucil) or methylcellulose (Citrucel) without a prescription. Ask your provider about these.
- Always talk to your provider before using any laxative medicines.
- You may use acetaminophen (Tylenol) for mild pain. Medicines such as aspirin, ibuprofen (Advil, Motrin), or naproxen (Aleve, Naprosyn) may make your symptoms worse. Talk to your provider about medicines you can use.
There are many types of medicines that can help prevent or treat attacks of your Crohn disease. Some of these are often started in the hospital.
When to Call the Doctor
Contact your provider if you have:
- Persistent or recurring cramps or pain in your lower stomach area
- Bloody diarrhea, often with mucus or pus
- Diarrhea that cannot be controlled with diet changes and medicines
- Weight loss (in everyone) and failure to gain weight (in children)
- Rectal bleeding, drainage, or sores
- Fever that lasts more than 2 or 3 days, or a fever higher than 100.4°F (38°C) without an explanation
- Nausea and vomiting that lasts more than a day
- Skin sores or lesions that do not heal
- Joint pain that keeps you from doing your everyday activities
- Side effects from any medicines prescribed for your condition
- An ostomy, and your ostomy site is red, swollen, hard, or bleeding
- Very little or no stool coming out of the ostomy
References
Ahmed M, Kinnucan JA, Farraye FA. Inflammatory bowel disease: Crohn disease and ulcerative colitis. In: Kellerman RD, Rakel DP, Heidelbaugh JJ, Lee EM, eds. Conn's Current Therapy 2024. Philadelphia, PA: Elsevier 2024:247-255.
Ananthakrishnan AN, Reguerio MD. Management of inflammatory bowel disease. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 116.
Crohn's & Colitis Foundation website. What is Crohn's disease? www.crohnscolitisfoundation.org/patientsandcaregivers/what-is-crohns-disease. Accessed December 5, 2024.
Lichtenstein GR. Inflammatory bowel disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 127.
-
Inflammatory bowel disease - illustration
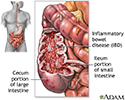
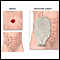
Crohn disease, also called regional enteritis, is a chronic inflammation of the intestines which is usually confined to the terminal portion of the small intestine, the ileum. Ulcerative colitis is a similar inflammation of the colon, or large intestine. These and other IBDs (inflammatory bowel disease) have been linked with an increased risk of colorectal cancer.
Inflammatory bowel disease
illustration
-
Inflammatory bowel disease - illustration
Crohn disease, also called regional enteritis, is a chronic inflammation of the intestines which is usually confined to the terminal portion of the small intestine, the ileum. Ulcerative colitis is a similar inflammation of the colon, or large intestine. These and other IBDs (inflammatory bowel disease) have been linked with an increased risk of colorectal cancer.
Inflammatory bowel disease
illustration
Review Date: 10/30/2024
Reviewed By: Jenifer K. Lehrer, MD, Gastroenterologist, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.