Depression in older adults
Depression in the elderlyDepression is a mental health condition. It is a mood disorder in which feelings of sadness, loss, anger, or frustration are present nearly every day for at least 2 weeks. They often interfere with daily life.
Depression in older adults is a widespread problem, and it is not a normal part of aging. It is often not recognized or treated.
Depression
Depression is feeling sad, blue, unhappy, or down in the dumps. Most people feel this way once in a while. Major depression is a mood disorder. It...

Causes
In older adults, life changes can increase the risk for depression or make existing depression worse. Some of these changes are:
- A move from home, such as to a retirement facility
- Chronic illness or pain
- Children moving away
- Spouse or close friends passing away
- Loss of independence (for example, problems getting around or caring for oneself, or loss of driving privileges)
Depression can also be related to a physical illness, such as:
- Thyroid disorders
-
Parkinson disease
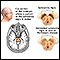
Parkinson disease
Parkinson disease results from certain brain cells dying. These cells help control movement and coordination. The disease leads to shaking (tremors...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Heart disease
-
Cancer
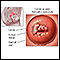
Cancer
Cancer is the uncontrolled growth of abnormal cells in the body. Cancerous cells are also called malignant cells.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Stroke
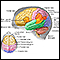
Stroke
A stroke occurs when blood flow to a part of the brain stops. A stroke is sometimes called a "brain attack. " If blood flow is cut off for longer th...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Dementia (such as Alzheimer disease)
Dementia
Dementia is a loss of brain function that occurs with certain diseases. It affects one or more brain functions such as memory, thinking, language, j...
 ImageRead Article Now Book Mark Article
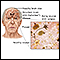
ImageRead Article Now Book Mark ArticleAlzheimer disease
Dementia is a loss of brain function that occurs with certain diseases. Alzheimer disease (AD) is the most common form of dementia. It affects memo...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Overuse of alcohol or certain medicines (such as sleep aids) can make depression worse.
Overuse of alcohol
Alcohol use disorder is when your drinking causes serious problems in your life, yet you keep drinking. You may also need more and more alcohol to f...
Symptoms
Many of the usual symptoms of depression may be seen. However, depression in older adults may be hard to detect. Common symptoms such as fatigue, appetite loss, and trouble sleeping can be part of the aging process or a physical illness. As a result, symptoms of early depression may be ignored, or confused with other conditions that are common in older adults. In severe cases, the symptoms may resemble dementia.
Exams and Tests
Your health care provider will perform a physical exam. Questions will be asked about your medical history and symptoms.
Blood and urine tests may be done to look for a physical illness.
A mental health specialist may be needed to help with diagnosis and treatment.
Treatment
The first steps of treatment are to:
- Treat any illness that may be causing the symptoms.
- Stop taking any medicines that may be making symptoms worse.
- Avoid alcohol and sleep aids.
If these steps do not help, medicines to treat depression and talk therapy often help.
Providers often prescribe lower doses of antidepressants to older people, and increase the dose more slowly than in younger adults.
To better manage depression at home:
- Exercise regularly, if your provider says it is OK.
- Surround yourself with caring, positive people and do fun activities.
- Learn good sleep habits.
- Learn to watch for the early signs of depression, and know how to react if these occur.
- Drink less alcohol and do not use illegal drugs.
Illegal drugs
Substance use is the continued use of alcohol, illegal drugs, or the misuse of prescription or over-the-counter medicines with negative consequences....
Read Article Now Book Mark Article - Talk about your feelings with someone you trust.
- Take medicines correctly and discuss any side effects with your provider.
Outlook (Prognosis)
Depression often responds to treatment. The outcome is usually better for people who have access to social services, family, and friends who can help them stay active and engaged.
The most worrisome complication of depression is suicide. Men make up most suicides among older adults. Divorced or widowed men are at the highest risk.
Suicide
Suicide is the act of taking one's own life on purpose. Suicidal behavior is any action that could cause a person to die, such as taking a drug over...

Families should pay close attention to older relatives who are depressed and who live alone.
When to Contact a Medical Professional
Contact your provider if you keep feeling sad, worthless, or hopeless, or if you cry often. Also call if you're having trouble coping with stresses in your life and want to be referred for talk therapy.
If you are caring for an aging family member and think they may have depression, contact their provider.
If you or someone you know is thinking about suicide, call or text 988 or chat 988lifeline.org. You can also call 1-800-273-8255 (1-800-273-TALK). The 988 Suicide and Crisis Lifeline provides free and confidential support 24/7, anytime day or night.
You can also call 911 or the local emergency number or go to the hospital emergency room. DO NOT delay.
If someone you know has attempted suicide, call 911 or the local emergency number right away. DO NOT leave the person alone, even after you have called for help.
References
American Psychiatric Association website. Persistent depressive disorder. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision (DSM-5-TR). Washington, DC: American Psychiatric Association Publishing; 2022.
Fava M, Mischoulon D, Cassano P, Papakostas GI, Stem TA. Depressive disorders. In: Stern TA, Wilens TE, Fava M, eds. Massachusetts General Hospital Comprehensive Clinical Psychiatry. 3rd ed. Philadelphia, PA: Elsevier; 2025:chap 28.
Fox C, Hameed Y, Maidment I, Laidlaw K, Hilton A, Kishita N. Mental illness in older adults. In: Fillit HM, Rockwood K, Young J, eds. Brocklehurst's Textbook of Geriatric Medicine and Gerontology. 8th ed. Philadelphia, PA: Elsevier; 2017:chap 56.
National Institute on Aging website. Depression and older adults. www.nia.nih.gov/health/depression-and-older-adults. Updated July 7, 2021. Accessed September 1, 2024.
US Preventive Services Task Force, Barry MJ, Nicholson WK, et al. Screening for depression and suicide risk in adults: US Preventive Services Task Force Recommendation Statement. JAMA. 2023;329(23):2057-2067. PMID: 26813211 pubmed.ncbi.nlm.nih.gov/26813211/.
-
Depression among the elderly - illustration
The elderly are at high risk for depression because they are more likely than younger people to have experienced illness, death of loved ones, impaired function and loss of independence. The cumulative effect of negative life experiences may be overwhelming to an older person.
Depression among the elderly
illustration
-
Depression among the elderly - illustration
The elderly are at high risk for depression because they are more likely than younger people to have experienced illness, death of loved ones, impaired function and loss of independence. The cumulative effect of negative life experiences may be overwhelming to an older person.
Depression among the elderly
illustration
Review Date: 7/17/2024
Reviewed By: Fred K. Berger, MD, addiction and forensic psychiatrist, Scripps Memorial Hospital, La Jolla, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.


